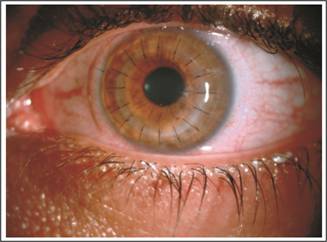
Fig. 1A: Anterior segment photograph after big bubble DALK
in Advance d Keratoconus 1 week follow up.
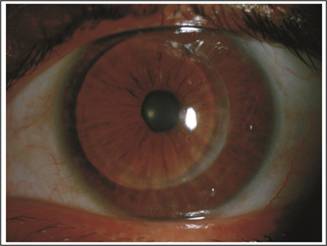
Fig. 1B: Post Big Bubble DALK anterior segment photograph in
advance keratoconus.
Original Article
Clinical Results of Deep
Anterior Lamellar Keratoplasty in Treatment of Advanced Keratoconus; Big Bubble
Technique
Bushra Akbar, Rana Intisar-ul-Haq,
Mazhar Ishaq, Paree Chera, Kashif Siddique
Pak J Ophthalmol 2017, Vol. 33 No. 1
. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .
. . . . . . . . . . . . . . . . . . . . . . . . .. . .. . . . . . . . . . . . .
. . . . . . . . . . . . . . . . . . . . . .
. .
Keratoconus is a degenerative, non-inflammatory
corneal ectatic disorder characterized by progressive central, paracentral
stromal thinning, protrusion and visual deterioration due to myopia, myopic
astigmatism and irregular astigmatism. Early to moderate cases of keratoconus
are managed with spectacles, rigid gas permeable contact lenses, providing
satisfactory visual rehabilitation and the disease progression can be effectively
halted by corneal collagen cross linking. However, keratoconus affects mainly
young working population, advanced cases requires surgical intervention due to
non satisfactory and intolerant fitting of contact lens, extreme corneal
thinning restricting the corneal cross linking or intracorneal ring segments, and
apical scarring in the visual axis, with a resultant very poor or unacceptable
vision1. Common surgical options include PKP and DALK. DALK is a
selective form of layered keratoplasty, which involves the removal and
replacement of diseased layers of cornea while retaining the recipient healthy
endothelium1,2,3. This preservation of endothelium minimized the
incidence of endothelial allograft rejection and concomitantly the dose and
duration of postoperative steroids administration and the complications
associated with its use2,3. PKP remained procedure of choice for all
keratoplasty indications for decades, despite its draw backs, largely due to
its superior visual outcomes and a longer surgical experience2,3,4.
Visual outcome is predominantly influenced by corneal transparency both in PKP
and DALK, however the visual recovery was significantly compromised in DALK by
scattering of light at donor host interface irregularity owing to residual
stroma adherent to descemet's membrane5,6. Many surgical
methodologies has been described for separation of stroma from descemet's
membrane and endothelium in DALK to achieve optimal interface, starting with
Barraquer microkeratome and Malbran ''peeling off technique” based on deep
stromal dissections7,8.
To the
best of our knowledge, this is the first study in Pakistan on clinical outcomes
of DALK using Anwar's big bubble technique in advanced keratoconus. We aim to
share our initial clinical experience in terms of refractive outcomes and
complications at 1 year after DALK using Anwar's big bubble technique in
Pakistani eyes with advanced keratoconus to generate local data and pave a way
for guidelines regarding surgical interventions in treatment of advanced
keratoconus in Pakistan.
METHODS AND MATERIALS
This quasi experimental
study enrolled consecutive patients of advanced keratoconus who underwent
successful DALK using Anwar's big bubble technique at Armed forces institute of
ophthalmology from November 2015 to Nov 2016 after approval of local ethical
committee. An informed consent was obtained from all the participants of study.
Inclusion criteria included patients with advanced keratoconus between 18 and
30 years of age. Advanced keratoconus was defined as grade 4 disease according
to the RETICS classification1 (Insufficient corneal thickness for
ICRS implantation or CXL with persistent contact/scleral lenses intolerance and
poor CDVA of 0.6). Exclusion criteria included eyes with corneal scarring and
opacity involving descement’s membrane and endothelium (healed hydrops) other
ocular co morbidity (amblyopic, strabismus, posterior segment pathology),
systemic diseases, neurological problems, or any topical or systemic
medications that may affect visual acuity, intraoperative complications
meriting a conversion to penetrating keratoplasty or failure to achieve big
bubble, requiring completion of DALK by lamellar dissection. Preoperative and
postoperative ocular examinations at 1, 6 and 12 months included UDVA, CDVA (measured
on Snellen visual acuity chart, converted to logMAR notation), SE, Ast, slit
lamp biomicroscopy and dilated fundus examination. Ocular investigations
included corneal topography (dual scheimpflug based corneal topography, Galilei
G4), specular microscopy (Topcon sp-3000, USA) for endothelial cell density
analysis and Anterior Segment Optical Coherence Tomography (ASOCT, Topcon
Maestro 2000, Japan) for assessment of trephination depth in superficial
corneal opacities.
DALK using Anwar's Big
Bubble technique was done by a single corneal surgeon in all patients under
general anaesthesia. The geometric center of the recipient cornea was marked
after draping and eye lid speculum insertion as per standard clinical
techniques. A partial thickness trephination of 8.0 mm (range 8.0 -8.50 mm)
diameter at predicated depth in corneal stroma (350 to 500 microns) was
achieved via MORIA suction trephine with Guard (MORIA, France) making sure
centration at all times. A 30-gauge needle, bent at 60 degrees 5 mm from the
tip with bevel facing down, attached to a 3 ml syringe was used to inject the
air, 3 to 4 cm from the entry site, into deep stroma to achieve big bubble,
that separates the stroma and the descemet's membrane, evidenced as a semi
opaque central disk with a sudden ease on resistance of the plunger. Deepest
stromal layers were gently dissected from center to periphery into 4 quarters
by angled blunt tipped Holland DALK scissors (DALK Set, Katena USA). These
dissected deep stromal layers were then excised with Holland DALK right and
left scissors (DALK Set, Katena, USA) to expose the clear and shiny descemet's
membrane. The wound edges were then trimmed as vertically as possible to
minimize post-operative astigmatism.
Donor corneas were procured
by hospital corneal and retrieval program and transported in McCarey- Kaufmann
medium. Donor corneas deemed fit based on negative infectious serology (HIV,
hepatitis) and optical clarity, were only used for DALK in our study. Donor
graft of 0.25 mm larger than recipient bed was trephined with endothelial side
up on Teflon block. The endothelium was stained with trypan blue and peeled off
with methylcellulose sponge. The donor graft was then sutured onto the
recipient bed with sixteen 10-0 nylon interrupted sutures (ALCON laboratories
USA).
Postoperatively, patients
were advised topical antibiotics moxifloxacin (vigamox, Alcon) 4 hourly and
topical steroids prednisolone acetate 1% (Predforte, Allergan) eye drops 6 hourly
gradually tapered over a period of 6 weeks. Suture removal and manipulation was
done between 24 to 27 weeks after 2nd postoperative exam at 6 months and suture
removal was completed till 12 months, one week prior to the last follow up exam
in all patients. Meanwhile, only loose or infected sutures were removed or
replaced if required.
Data
analysis was done using SPSS version 20. Quantitative data was described as
mean ± standard deviation and nominal data as frequencies. Paired sample t-
test was used to analyze change in the parameters over baseline at post
-operative test points of 1, 6 and 12 months. p value of <0.05 with 95% confidence interval was considered
statistically significant.
RESULTS
Seventeen eyes of 17 patients were included in this
study who underwent DALK using big bubble technique and completed a minimum
follow up of 12 months. Big bubble was achieved in (94.11%) 17/18 of eyes. Two
eyes were excluded from the study due to failed big bubble (5.88%) 1/18 with
subsequent manual stromal lamellar dissection in one eye and an intraoperative macro
perforation requiring conversion to PKP in the other eye. No other
intraoperative or postoperative complication was recorded.
The mean age was 26.29 ± 10.40 years. There were 13
(76.47%) males and 4 (23.53%) females. Suture manipulation was done in 3 eyes
and mean suture manipulation time was 25.588 ± 1.325 (range 24 – 28) weeks. The
mean suture removal time was 11.555 ± 0.472. Mean baseline logMAR UDVA was
1.376 ± 0.286 which significantly improved over all postoperative test points
of 1, 6 and 12 months with a final UDVA of 0.964 ± 0.183 at 1 year. (p = 0.001, 0.000, 0.000 respectively)
Table 1. Mean baseline logMAR
CDVA 1.211 ± 0.228 improved significantly at all predetermined test points to a
mean logMAR CDVA of 0.647 ± 0.279 (p = 0.000,
0.000, 0.000 respectively) at 12 months
Table 1. The mean pre op SE -3.806 ± 1.358 and Ast-3.205 ± 2.653 although
showed a reduction over post-operative test points but it was not significant (p > 0.05) except for a postoperative
astigmatism at 1 year (p = 0.010). Table 1. ECD evaluated by specular
microcopy did not show any significant loss over the postoperative follow up (p = 0.082) Table 1. No signs of endothelial decompensation or rejection were
reported in any eye over 1 year follow up in our study.
Table 1: Refractive Results after deep Anterior Lamellar
Keratoplasty using ANWAR’S big bubble technique.
|
Study Parameters |
PREOPERATIVE |
POST OPERATIVE |
||
|
Mean ± SD |
|
1 MONTH |
6 MONTHS |
12 MONTHS |
|
UDVA (logMAR) |
1.376 ± 0.286 |
1.079 ± 0.331 |
1.061 ± 0.263 |
0.964 ± 0.183 |
|
p Value |
|
0.001* |
0.000* |
0.000* |
|
CDVA(logMAR) |
1.211 ± 0.228 |
0.982 ± 0.174 |
0.782 ± 0.237 |
0.647 ± 0.279 |
|
p Value |
|
0.000* |
0.000* |
0.000* |
|
SE(D) |
-3.806 ± 1.358 |
-4.741 ± 1.150 |
-4.080 ± 2.432 |
-3.092 ± 2.420 |
|
p Value |
|
0.325 |
0.864 |
0.330 |
|
AST(D) |
-3.205 ± 2.653 |
-3.455 ± 0.806 |
-3.161 ± 0.905 |
-2.088 ± 1.441 |
|
p Value |
|
0.869 |
0.836 |
0.010* |
(*) p Value<0.05,
Paired sample t test

Fig. 1A: Anterior segment photograph after big bubble DALK
in Advance d Keratoconus 1 week follow up.

Fig. 1B: Post Big Bubble DALK anterior segment photograph in
advance keratoconus.
DISCUSSION
Archila, in 1985, performed stromal dissection with
aid of 1 cc air injection above the descemet's membrane, with subsequent
spatula dissection of overlying recipient stroma9. Sugito and Kundo
introduced hydro delamination of residual stromal fibers followed by
delamination of hydrated stromal fibers from the descemet's membrane10.
Melles et al conceptualized the technique of lamellar dissection depth by
exchanging aqueous with air and creating an optical air endothelium interface,
that acts as convex mirror and reflects the depth of instrument in stroma
coupled with viscodissection of lamellar plane to bare descemet’s membrane11,12.
Anwar and Teichmann described the famous big bubble technique, where a large
air bubble facilitates the separation of descemet's membrane from stroma after
initial partial stromal trephination with resultant optimal interface, totally
baring descemet's membrane13. This limited post-operative interface
haze, provided excellent visual results, early visual rehabilitation in
keratoconus14. Despite its steep learning curve and technical
challenges, clinically significant advantages of Anwar’s big bubble DALK has
shifted the paradigm from PKP to DALK amongst corneal surgeons across the
globe for endothelium and descemet’s membrane sparing
corneal disorders13-17. However very few tertiary care centers in Pakistan are offering selective layered
keratoplasties at present in contrast to other developing countries of south
east Asia15,16.
Keratoconus has been the leading indication for
keratoplasty in many populations and geographical zones in the last few
decades. This paradigm shift in indications has been probably the outcome of
developmental state and socioeconomic profile of population, clinical
significant advantages of DALK and improvement of eye banks and surgical
sophistication18.19,20. We performed DALK in seventeen eyes of
advanced keratoconus using big bubble technique with a 1-year post-operative
follow up. Big bubble was achieved in 17 (94.1%) eyes out of 18 eyes and only
one eye 5.88% required layer by layer stromal dissection that was comparable to
or better than similar studies13-17. Only one eye (5.88%) required
conversion to PKP due to intraoperative macro perforation. Anwar in his study
reported perforation in 16 (9%) eyes out of 181 eyes and conversion to PKP in
one eye, Feizi et al reported a conversion rate of 2.3% in 103 eyes. This
success rate of big bubble formation and conversion rate in our study can be considered
acceptable for a being beginners in challenging surgical learning curve13,14.The
mean gain in UDVA and CDVA from 1.1376 ± 0.286 to 0.964 ± 0.18 and 1.211 ±
0.228 to 0.647 ± 0.279 one year in our study is comparable to results reported
by Feizi et al14. Gain of more than 3 Snellen lines in
CDVA was achieved in 94.44% of eyes similar to gain of more than 2 lines in 91%
of eyes reported by Danosoury23. A CDVA of 20/70 in 40% and 20 /40
in 30% of eyes was achieved as compared to
20 /40 or better achieved in 77.8% of eyes in similar clinical trials of
DALK using big bubble technique14. Similarly the SE and Ast showed
reductions over the follow up test points14. In current study,
astigmatism of more than 4 D in 17% of eyes was documented in accordance with
high post DALK Ast in 26% of eyes in previous similar trials at 1 year that was
managed with relaxing incisions and adjustment sutures14. These
differences in refractive results and post DALK refractive error in our study
compared to previous similar clinical studies in international studies may be
explained by variations in factors affecting post DALK refractive status like
suturing techniques, mean time of suture removal, suture manipulation for high
cylindrical errors, refraction at variable duration after suture removal and
our limited surgical expertise21,24. Moreover the quality of vision
can also be negatively affected by interface haze even if stroma fully excised
and no interface haze is detectable on slit lamp22. This can be seen
as selective stromal reflectivity on confocal microscopy and decreased contrast
sensitivity6. The reason being not completely understood and
speculated to be excessive healing response22. No case of
subepithelial or stromal graft rejection or endothelial cell was reported in
this study which was less than reported
immunologic rejection of 3 to 8% after DALK, and 14.3% reported by Feizi et al6,24,25.
This may be attributed to our careful patient selection excluding allergic co-morbidities,
explained by Feizi et al in his study, that led us to an obvious advantage of
early tapering of steroids and no complications post operatively of raised
intraocular pressures. Lu et el26 have shown that DALK with big
bubble technique using femto laser is a new safe, effective and accurate
technique for treating patients having keratoconus.
The major limitations of this study is a small
sample size, relatively shorter duration of follow. We strongly feel that large
prospective multi center trials on big bubble DALK recruiting larger number of
advanced keratoconus patients with a long term follow up to increase surgical
experience and will help to generate standardized data on clinical results,
recurrence of disease and factors predicting refractive outcomes in our
population. DALK using Anwar’s big bubble technique has shown lesser
complications in terms of endothelial rejection and endothelial cell loss, with
satisfactory refractive results in young keratoconus patients, and we recommend
it to be a preferred surgical technique over penetrating keratoplasty, despite
its technical challenges and steep surgical learning curve.
CONCLUSION
DALK using Anwar's big bubble technique has shown
lesser complications in terms of endothelial rejection and edothelial cell loss
with satisfactory refractive results in young keratoconus patients and we
recommend it to be a preferred surgical technique over penetrating
keratoplasty, despite its technical challenges and steep surgical learning
curve.
Author’s Affiliation
Dr.
Bushra Akbar
Department of Ophthalmology,
Armed Forces Institute of Ophthalmology, Rawalpindi, Pakistan
Dr. Rana
Intisar-ul-Haq
Department of
Ophthalmology, Armed Forces Institute of Ophthalmology, Rawalpindi, Pakistan
Dr.
Mazhar Ishaq
Department of
Ophthalmology, Armed Forces Institute of Ophthalmology, Rawalpindi, Pakistan
Dr.
Paree Chera
Department of
Ophthalmology, Armed Forces Institute of Ophthalmology, Rawalpindi, Pakistan
Dr.
Kashif Siddique
Statistician,
Research (Academic Affairs), King Salman Armed Forces Hospital, KSA
Role of Authors
Dr. Bushra Akbar
Study design, Data acquisition, interpretation, and
analysis of data, manuscript drafting.
Dr. Intisar-ul-Haq
Study design,
critical review.
Dr. Mazhar Ishaq
Critical review.
Dr. Paree Chera
Data collection, interpretation and manuscript
drafting
Dr. Kashif Siddique
Study design, interpretation, analysis of data and
critical review
REFERENCES
1.
Arnalich-Montiel F, Alió del Barrio JL, Alió JL. Corneal surgery in keratoconus: which type, which technique,
which outcomes? Eye and Vision. 2016; 3(2); 1-14.
2.
Terry M. The Evolution of Lamellar Grafting
Techniques Over Twenty-five Years. Cornea, 2000; 19 (5): 611-616.
3.
Funnell C, Ball J, Noble B. Comparative cohort study of the outcomes of deep lamellar
keratoplasty and penetrating keratoplasty for keratoconus. Eye. 2005; 20 (5):
527-532.
4.
Jones M, Armitage W, Ayliffe W, Larkin D, Kaye S. Penetrating and Deep Anterior Lamellar
Keratoplasty for Keratoconus: A Comparison of Graft Outcomes in the United
Kingdom. Investigative Opthalmology & Visual Science, 2009; 50 (12): 5625-9.
5.
Fontana L, Parente G, Sincich A, Tassinari G. Influence of Graft–Host Interface on the Quality of Vision After
Deep Anterior Lamellar Keratoplasty in Patients with Keratoconus. Cornea, 2011;
30 (5): 497-502.
6.
Feizi S, Javadi M, Rastegarpour A. Visual Acuity and Refraction after Deep Anterior
Lamellar Keratoplasty with and Without Successful Big-Bubble Formation. Cornea,
2010; 29 (11): 1252-1255.
7.
Barraquer J. Lamellar keratoplasty (special techniques). Ann
Ophthalmol. 1972; 4: 437–469.
8.
Polack F. Lamellar keratoplasty: Malbran’s “peeling off”
technique. Arch Ophthalmol. 1971; 86: 293-296.
9.
Archila E. Deep lamellar keratoplasty dissection of host
tissue with intrastromal air injection. Cornea, 1985; 3: 217-218.
10. Sugita J, Kondo J. Deep lamellar keratoplasty with complete removal of pathological stroma
for vision improvement. Br J Ophthalmol. 1997; 81: 184-188.
11. Melles G, Rietveld F, Beekhuis W, Binder P. A Technique to Visualize Corneal Incision and
Lamellar Dissection Depth During Surgery. Cornea, 1999; 18 (1): 80-86.
12. Melles G, Lander F, Rietveld F, Remeijer L, Beekhuis W, Binder P. A new surgical technique for deep stromal,
anterior lamellar keratoplasty. The British Journal of Ophthalmology, 1999; 83
(3): 327-333.
13. Anwar M, Teichmann KD. Big-bubble technique to bare Descemet‘s membrane in anterior lamellar
keratoplasty. J Cataract Refract Surg. 2002; 28: 398-403.
14. Feizi S, Javadi M, Jamali H, Mirbabaee F. Deep Anterior Lamellar Keratoplasty in Patients
with Keratoconus: Big-Bubble Technique. Cornea, 2010; 29 (2): 177-182.
15. Tan DTH, Mehta JS. Future of lamellar corneal transplantation. Cornea, 2007; 26: S21-S28.
16.
Fogla R. Deep anterior lamellar keratoplasty in the
management of keratoconus. Indian Journal of Ophthalmology, 2013; 61 (8): 465-8.
17.
Söğütlü Sarı E, Kubaloğlu A, Ünal M, Piñero Llorens D,
Koytak A, Ofluoğlu A et al. Penetrating keratoplasty versus deep
anterior lamellar keratoplasty: comparison of optical and visual quality
outcomes. British Journal of Ophthalmology, 2012; 96 (8): 1063-1067.
18. de Sanctis U, Alovisi C, Baucheiro L,
Caramello G et al. Changing trends in
corneal graft surgery: a ten-year review. Int J Ophthalmol. 2016; 9 (1): 48-52.
19.
Rezaei Kanavi M, Javadi M, Motevasseli T, Chamani T, Rezaei
Kanavi M, Kheiri B et al. Trends in indications and techniques
of corneal transplantation in Iran from 2006 to 2013; an 8-year review. J
Ophthalmic Vis Res. 2016; 11 (2): 146.
20.
Altay Y, Burcu A, Aksoy G, Singar Ozdemir E, Ornek F. Changing indications and techniques for corneal transplantations
at a tertiary referral center in Turkey, from 1995 to 2014. Clinical
Ophthalmology, 2016; 10: 1007-1013.
21.
Javadi M, Feizi S, Mirbabaee F, Rastegarpour A. Relaxing
Incisions Combined With Adjustment Sutures for Post-Deep Anterior Lamellar
Keratoplasty Astigmatism in Keratoconus. Cornea, 2009; 28 (10): 1130-1134.
22.
Feizi S, Javadi M, Mohammad-Rabei H. An Analysis of Factors Influencing Quality of Vision after
Big-Bubble Deep Anterior Lamellar Keratoplasty in Keratoconus. American Journal
of Ophthalmology, 2016; 162: 66-73.
23. Cheng Y, Visser N, Schouten J, Wijdh R, Pels E, van Cleynenbreugel H et
al. Endothelial
Cell Loss and Visual Outcome of Deep Anterior Lamellar Keratoplasty versus
Penetrating Keratoplasty: A Randomized Multicenter Clinical Trial.
Ophthalmology, 2011; 118 (2): 302-309.
24. El-Danasoury A. Big Bubble Deep Anterior Lamellar Keratoplasty (BB-DALK).
International Ophthalmology Clinics, 2013; 53 (1): 41-53.
25. Feizi SJavadi M. Factors Predicting
Refractive Outcomes after Deep Anterior Lamellar Keratoplasty in Keratoconus.
American Journal of Ophthalmology, 2015; 160 (4): 648-653.
26. Lu Y, Chen X, Yang L, Xue C, Huang Z. Femtosecond laser assisted
deep anterior lamellar keratoplasty with big-bubble technique for keratoconus.
Indian J Ophthal 2016; 64(9): 639-642.